Blood, infertility and death: The struggle to save the lives of mothers and babies in Mozambique
Fatima Abacassamo has witnessed first-hand the devastating effects of the withdrawal of international aid by the United States and other Western nations on vulnerable pregnant women and newborn babies in Niassa, a remote and poor province far north of Mozambique.
As head of Mozambique programming for EngenderHealth, which assists pregnant women facing complications in Niassa, Abacassamo is at pains to explain how maternal health care services have nearly ground to a halt in this province.
“Many women in Niassa are now reaching health facilities only when complications have already developed,” Abacassamo says in an interview. “A lot of pregnant women now require urgent surgical intervention, which is not always available and is far away, rather than planned care, which allows for timely preparation to save lives.”
For three years, and with $6.74 million (£5m) in funding from the United States Agency for International Development (USAID), EngenderHealth implemented community-based maternal services that helped identify high-risk pregnancies and map and monitor access to health facilities before the onset of labour.
But at the stroke of a pen a year ago, Donald Trump essentially shut down USAID, with other Western nations such as the UK, Germany and France also stopping funding for overseas development programs. Now, poor and vulnerable would-be mothers in Niassa and elsewhere across Mozambique have been left stranded and unable to access life-saving services and procedures.
This has seen EngenderHealth halt all activities related to maternal health service delivery in health facilities in Niassa. It has also stopped training programs for healthcare providers and community-based awareness activities.
“In the province we used to serve [Niassa], pregnant women now arrive at health facilities with complications such as high blood pressure, excessive bleeding and in some instances cases where the placenta covers the cervix. These can result in death or long-term disabilities, such as prolonged labour or infertility due to uterine rupture, often caused by delayed access to appropriate surgical interventions, Abacassamo says. She adds that “the lack of timely access to safe cesarean sections performed by trained medical personnel in emergency situations is a critical and worsening” gap in maternal healthcare in Niassa.
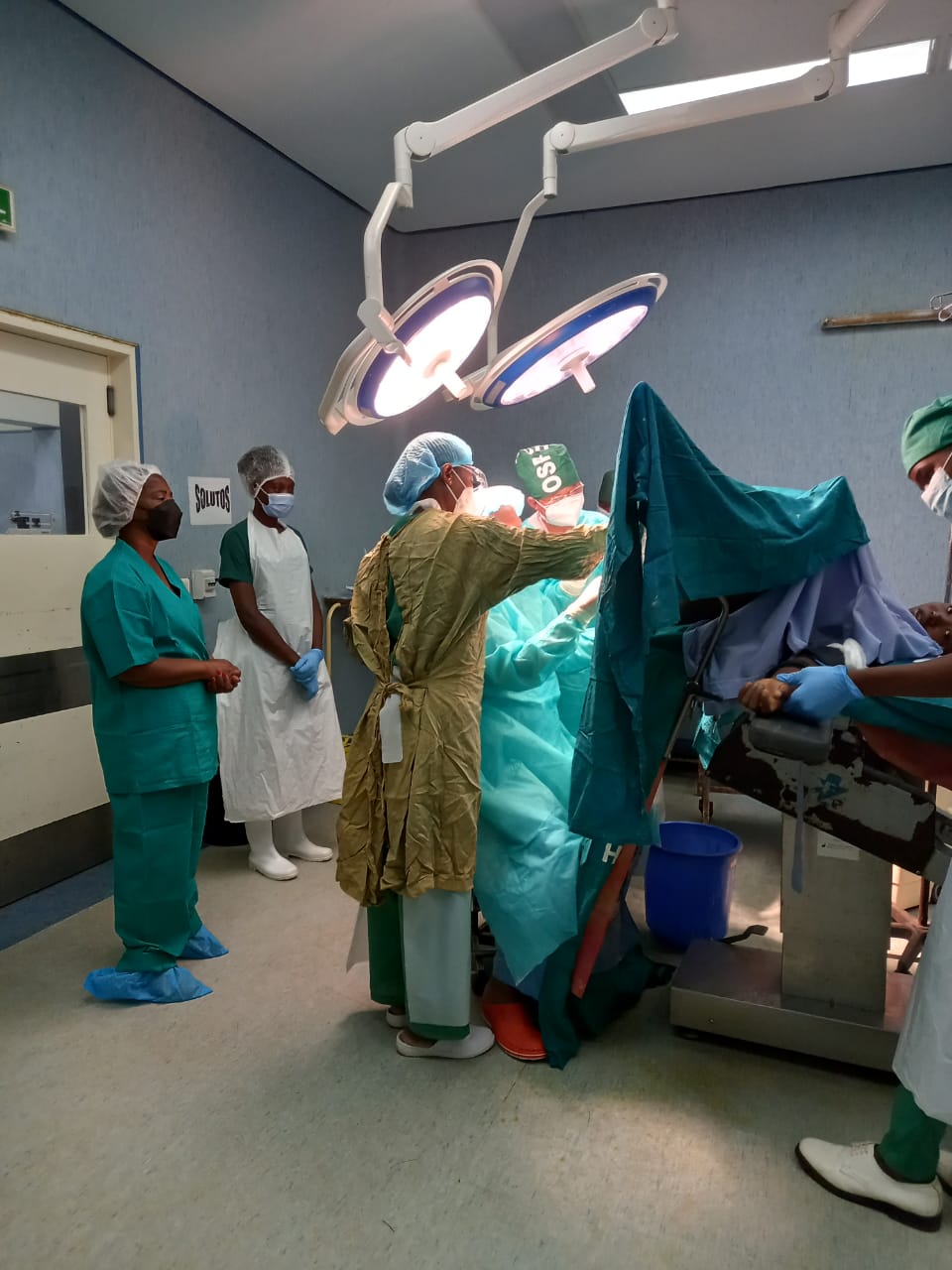 open image in gallery
open image in galleryAbacassamo worries that “delays in access to timely maternal health services, limited early detection of risk during pregnancy, and gaps in referral and preparedness” systems will result in a sharp spike in maternal deaths.
Any gains that Mozambique has made in reducing maternal deaths and infant morbidities in recent years are at risk thanks to this “change in the donor landscape,” especially the withdrawal of funding by donor organisations, Nelida Rodrigues, the representative in Mozambique for the UN Population Fund (UNFPA), tells The Independent.
Rodrigues explains that in the same province of Niassa, several mobile clinics have ceased, and community outreach programmes halted, while last-mile distribution of life-saving commodities may become inconsistent due to the withdrawal of international development aid by USAID and other organisations.
Throughout Mozambique, less than half of women (48.6 per cent) receive the recommended four or more antenatal care visits from health providers, the United Nations’ World Health Organisation (WHO) says. Only 36 per cent of women and 41 per cent of newborns in Mozambique receive a postnatal consultation within the first two days after birth.
This is despite improvements in the country’s infant mortality, which has declined from 54 deaths per 1,000 live births in 1997 to 24 per 1,000 live births in 2022/2023. Mozambique’s maternal mortality ratio had also halved, falling from 690 per 100,000 live births in 1997 to 233 per 100,000 live births in 2022/2023, according to the WHO.
“Recent reductions in funding for maternal and child health programmes are undermining the sustainability of key interventions in Mozambique. Cuts to financing for essential medicines, supply chains, and critical medical equipment are compromising the delivery, quality, and continuity of maternal and neonatal health services, posing a risk to the gains achieved in recent years,” a spokesperson for WHO in Mozambique says.
 open image in gallery
open image in gallery‘Maximising the impact of every dollar’
Community members and coordinators with health programmes in Niassa province tell The Independent that the halting of the EngenderHealth programme had left pregnant women and new mothers stranded in many districts of the province. Meanwhile, many new mothers are still waiting for follow-up operations and treatment procedures after giving birth in the past few months.
One community member says: “In villages on the banks of Niassa River, home births are still prevalent due to the distance and the need to cross Lake Niassa by boat. It could have been worse but we have matrons who were trained by EngenderHealth, and they assist with basic care, but when there are complications, it becomes a very difficult situation.
Other humanitarian organisations active in Mozambique, such as ActionAid, are also seeing funding reduced. Clotilde Noa, who works for ActionAid in Mozambique, says that this includes a shortage of medicines, a lack of equipment and materials for normal and caesarean deliveries and less anaesthesia materials.
Noa says ActionAid has been receiving requests for funding to support maternal health programs in Mozambique, mainly from local organisations and district governments.”
"In addition to the withdrawal of USAID, Mozambique is prone to natural disasters and has suffered an impact on health infrastructure when there are cyclones and floods,” Noa adds.
 open image in gallery
open image in galleryFaced with aid reductions and delays, development organisations in Mozambique are now rethinking their approach. The WHO office in Mozambique says it has now shifted focus towards sustainable approaches that improve efficiency and foster the integration of reproductive, maternal, newborn, and child health (RMNCH) services. This includes scaling up integrated, community-based programmes and strengthening primary health care facilities as the backbone of the health system.
It is also expanding access to family planning and reproductive health services, including contraception and counselling.
The WHO in Mozambique says it is “essential to support birth spacing and prevent unintended and high-risk early pregnancies” as a strategy to manage complications.
The UNFPA too is adapting its strategy to ensure “sustainability of maternal health services” through deeper collaboration and engagement with non-traditional donor countries, such as South Korea and Ireland, and exploring regional African collaborations.
“We are also further integrating maternal health with climate resilience... to maximise the impact of every dollar, and strengthening the capacity of domestic NGOs and provincial health authorities,” explained Rodrigues.
However, mobilising domestic resources for the health sector in Mozambique remains challenging, especially at a time when the country’s finances are precarious. Mozambique’s economy remains susceptible to the effects of climate change, with frequent cyclones undermining growth in the dominant agricultural sector, which accounts for about 25 per cent of GDP.
For its part, EngenderHealth is seeking secure funding and is exploring partnerships to provide technical assistance to other organisations Niassa and elsewhere in the country.
Abacassamo said: “If no funding is secured in the coming months, there is a possibility that the organisation may have to withdraw [from Mozambique]."
This article has been produced as part of The Independent’s Rethinking Global Aid project
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
CommentsСхожі новини

'Bizarre': Former student of White House shooting suspect says Cole Allen seemed like a completely average guy
Hormuz crisis throws spotlight on world's largest 'chokepoint' — the Malacca Strait

Mali violence escalates: Defence minister Sadio Camara killed in 'terrorist attack'
